 What is the role of healthy kidneys?
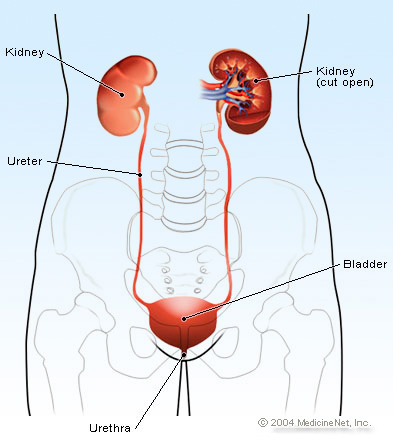
What is the role of healthy kidneys?
Most people think that the kidneys just make urine, but there is a lot more going on that affects many areas of the body. A health kidney is responsible for:
• Cleaning blood
• Producing urine
• Regulating blood pressure
• Balancing fluids, minerals and chemicals in the body
• Signalling the bones to make red blood cells
The following signs, symptoms and conditions indicate that it would be a good idea to visit a doctor and ask for a kidney check:
• Diabetes
•High blood pressure
• Family history of kidney disease
changes in urination including:
• Going more frequently or less often
•Colour becoming darker
• Foamy or bubbly
• feeling tired
•feeling weak
•feeling cold all the time
•shortness of breath
•swelling in face, feet or hands
• nausea or vomiting
• loss of appetite
• metallic taste in the mouth
• not wanting to eat meat
• mental confusion
People with diabetes or high blood pressure should be aware of their risk of developing kidney disease, as these are the top causes of CKD. When diabetes and high blood pressure are not controlled, they can cause damage to the tiny vessels throughout the body, including the nephrons in the kidneys.
Those with a family history of kidney disease are also at increased risk of developing chronic kidney disease.
In addition to being at greater risk for diabetes and high blood pressure, which can run in families and progress to kidney disease, there is a hereditary kidney disease called polycystic kidney disease (PKD). PKD is passed from one or both parents to their children. With polycystic kidney disease, fluid- filled cysts grow on the kidneys and can impede their ability to function.
These diseases cause damage to the glomeruli in the nephrons. When enough of the glomeruli in the nephrons are destroyed, chronic kidney disease can lead to end stage renal disease (ESRD) or kidney failure. It is at this point that either dialysis or a transplant is needed.
How to help prolong kidney function & prevent kidney failure
When someone is diagnosed with chronic kidney disease, the first step is to determine the stage of the disease.
The National Kidney Foundation has classified five stages to help doctors better treat their patients based on how much kidney function the patient has left. Measuring a person’s glomerular filtration rate (GFR) indicates how much blood is being filtered through the kidneys.
• Stage 1: GFR > 90 milliliter/ minute is CKD with normal or high GFR
• Stage 2: GFR = 60-89 ml/ min is mild CKD
• Stage 3: GFR = 30-59 ml/ min is moderate CKD
• Stage 4: GFR = 15-29 ml/ min is severe CKD
• Stage 5: GFR <15 ml/min is end stage renal disease (ESRD) or kidney failure.
During the first two stages of kidney disease a doctor may recommend limiting protein in the diet, controlling blood sugar and blood pressure levels, stopping smoking, exercising and practicing overall healthy habits.
In stage three of chronic kidney disease a visit to a nephrologist (doctor who specializes in kidney care) is recommended. In addition to following the advice given for people in stages one and two, the nephrologist may also refer the patient to a dietician for additional guidance in getting proper nutrition. Some people begin to feel some of the effects of kidney function loss in stage three.
By stage four people the nephrologist will explain the treatment options including dialysis and transplantation. If the patient will be on dialysis, the doctor will explain the different types of dialysis treatments available such as haemodialysis and peritoneal dialysis, and prepare for the patient to get an access — local where dialysis occurs.
At stage five the kidneys no longer function well enough to keep a person alive, so dialysis or a transplant must be done. The best access choice is a fistula, which should be placed a few months before dialysis treatment begins.
(Pamphlet information received from Dialysis Patient Citizens Inc. Submitted by Health Solutions Inc.)





